Table of Contents
Name of Procedure
- Diagnostic Thoracic Medial Branch Block (TMBB)
- Therapeutic Thoracic Medial Branch Block (TMBB)
Sample Opnote
Goal
To block and/or administer medications to the medial branch nerves that innervate the facet joints of the thoracic spine.
Indications
A diagnostic medial branch block might be performed to ameliorate pain from facet joints temporarily by using local anesthetic agents. The temporary block provides diagnostic value because a temporary relief in pain can help to determine if the treated facet joints are the source of the patient’s pain. This in turn can be used as part of a double comparative set of diagnostic blocks to move onto a radiofrequency ablation of the medial branch nerves.
A therapeutic medial branch block might be performed to ameliorate pathology around the medial branch nerves themselves, such as if a patient develops neuritis of the medial branch nerves after radiofrequency ablation/rhizotomy.
Contraindications
- Common contraindications
- Posterior fusion at the same levels as the target facet joints (ie, avoid L4-L5 facet treatment in a patient with a fusion at L4-L5) (…)
Anatomy
Overview
A “medial branch” technically refers to the medial branch of the dorsal ramus of a spinal nerve. This medial branch also innervates the multifidus muscle, which is of particular importance when performing a medial branch ablation.
The source/path/naming/innervation of the medial branch nerves and their target injection sites can be confusing so keep a few things in mind:
- Each facet joint is innervated by 2 medial branch nerves. In the lumbar spine, a joint is innervated by a branch from its top level and from the level above it. For example, an L4-L5 facet joint is innervated by a branch from the L3 and L4 spinal nerve.
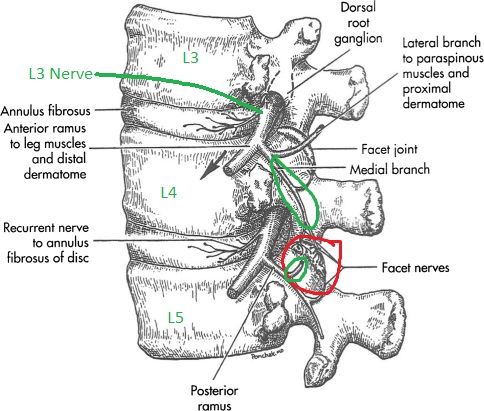
L4-L5 facet in red. L3 and L4 originating branches in green going to innervate that joint.
- The medial branch nerves run over the junction of the transverse process (TP) and superior articulating process (SAP) on the posterior side of the spine, at ONE LEVEL BELOW where it originates.
- See the L3 branch circled in green: to block the medial branch from L3 you target the TP and SAP at L4.
- Note how that branch innervates the L3-L4 joint and continues down to innervate the L4-L5 joint (red). So a block at the L3 level affects two joints.
- Likewise for the branch from L4, you block at L5.
- Now, put together the originating branches and their target sites to determine how to block a specific facet joint:
- To block the medial branch nerves that innervate the L4-L5 facet joint, you would target the junction of the TP and SAP at L4 and again at L5.
- Note this common pattern extends to multiple levels. To block 3 joints (L2-L3, L3-L4, L4-L5), your target sites will be at L2, L3, L4, L5. Note that at L3 and L4, you are getting two half joints at once, which simplifies our procedure.
Naming Notes
The images below use numbering based on the vertebral BODY that is being treated. Ie, a needle on the L4 transverse process is referred to as a L4 MBB target, which is different than the way the nerves would be labeled. This is done to make it easy to follow along with which vertebral bodies are leveled off and targeted.
Equipment/Skills/Setup
Core Equipment/Disposables: See our disposables/equipment article for “core” items that are common to all procedures.
Core Skills: See our guides to obtain images of the cervical, thoracic, or lumbar spine. Then steer a needle to direct it under the skin.
Special items and suggested setup for this procedure:
- 25g x 1.5″ hypodermic needle as your primary needle
- 5cc local anesthetic (1% lidocaine or 0.5% bupivacaine) in 10cc syringe as primary injectate
Landmarks and Patient Positioning
Position the patient in a basic prone position so that the bottom of the c-arm can go under the table below the area of the spine that is being treated.
Technique
For the sake of this tutorial we will assume we are treating the T9-T10, T10-T11, T11-T12 facet joints on one side, which means we have targets at the junction of the SAP and TP at T9, T10, T11, T12.
Steps:
- Obtain an AP or oblique/scotty dog view of T12, which will be the first target.
- Use your pointer to set an insertion site just above the TAP/SAP junction of T12. Insert your hypodermic needle right above the target and simply use a “down the barrel” approach to go straight down to the target.
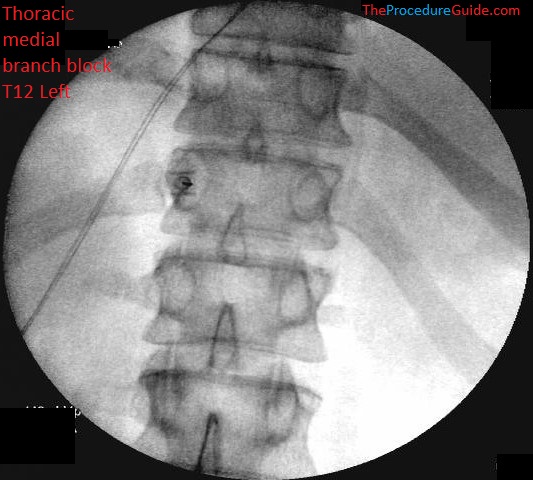
- Once on bone, confirm your depth on a lateral view
- Confirm that you do not appear to be beyond the transverse process or at the depth of the neuroforamina.
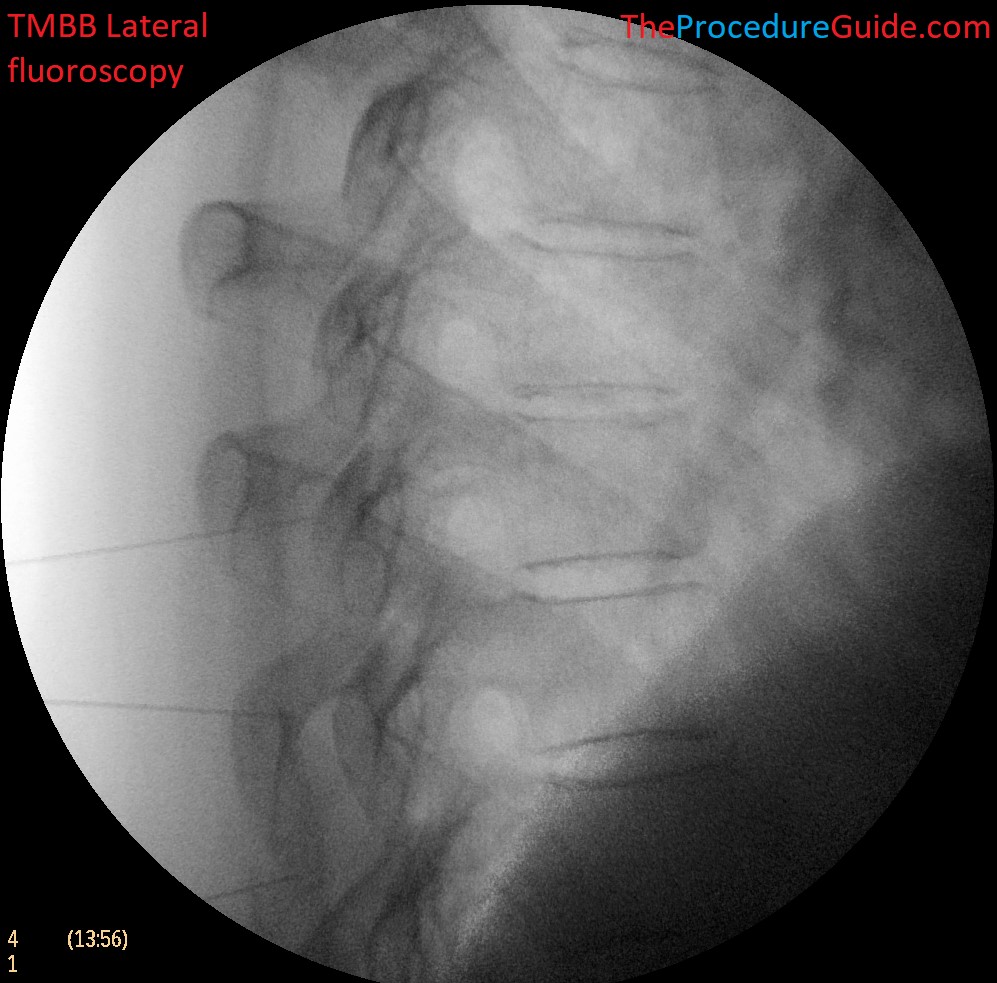
- Repeat steps 1-3 for each level being treated. (Remember to level of the vertebral body at the level that you’re targeting)
Tips
- ANATOMICAL NOTE: As you progress up the thoracic spine the medial branch nerves sit more lateral on the transverse process so you’re target is a bit lateral compared to lumbar levels.
- NEEDLE CHOICE: The thoracic spine is fairly superficial in many thin patients, so you can often get to it with a basic 25g x 1.5″ hypodermic needle.
- This way you don’t have to use a quincke needle, and since you’re just using a 25g you probably don’t need to anesthetize the skin (it’s the same needle you would use to anesthetize so instead of doing 2 pokes with the same needle, just do the one poke).
- Also, you probably don’t need a bent needle since you’re traveling a short distance.
- COUNTING LEVELS: In the thoracic spine it can get confusing which level you’re at if you don’t have a frame of reference:
- In the example above, after injecting at T12, leave the needle there while placing a pointer at T11.
- Take an image.
- This way you have a needle sitting at T12 (to act as a frame of reference) while pointing at T11.
- You can keep continuing this as far up as needed even when you no longer see the bottom or top of the rib cage.
- DEPTH AND SAFETY: If you enter skin right on top of the TP and go “down the barrel” till contacting TP, it is unlikely you can move to a dangerous depth.
- This means you probably don’t need a lateral after every image. As soon as you contact bone, you’ll know you’re at your target.
Sample Images
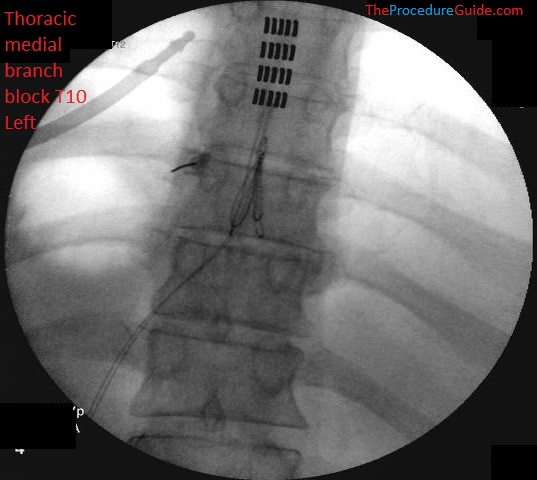
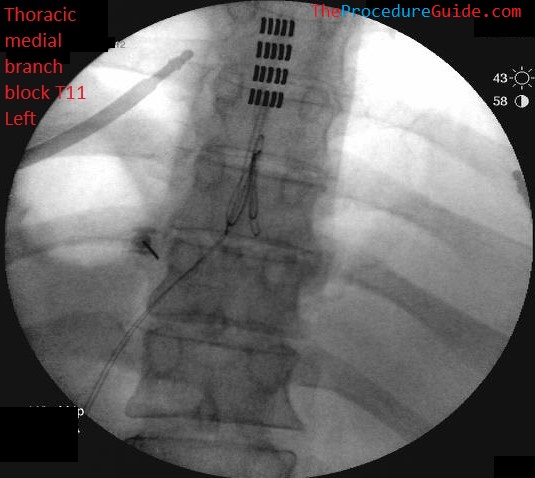
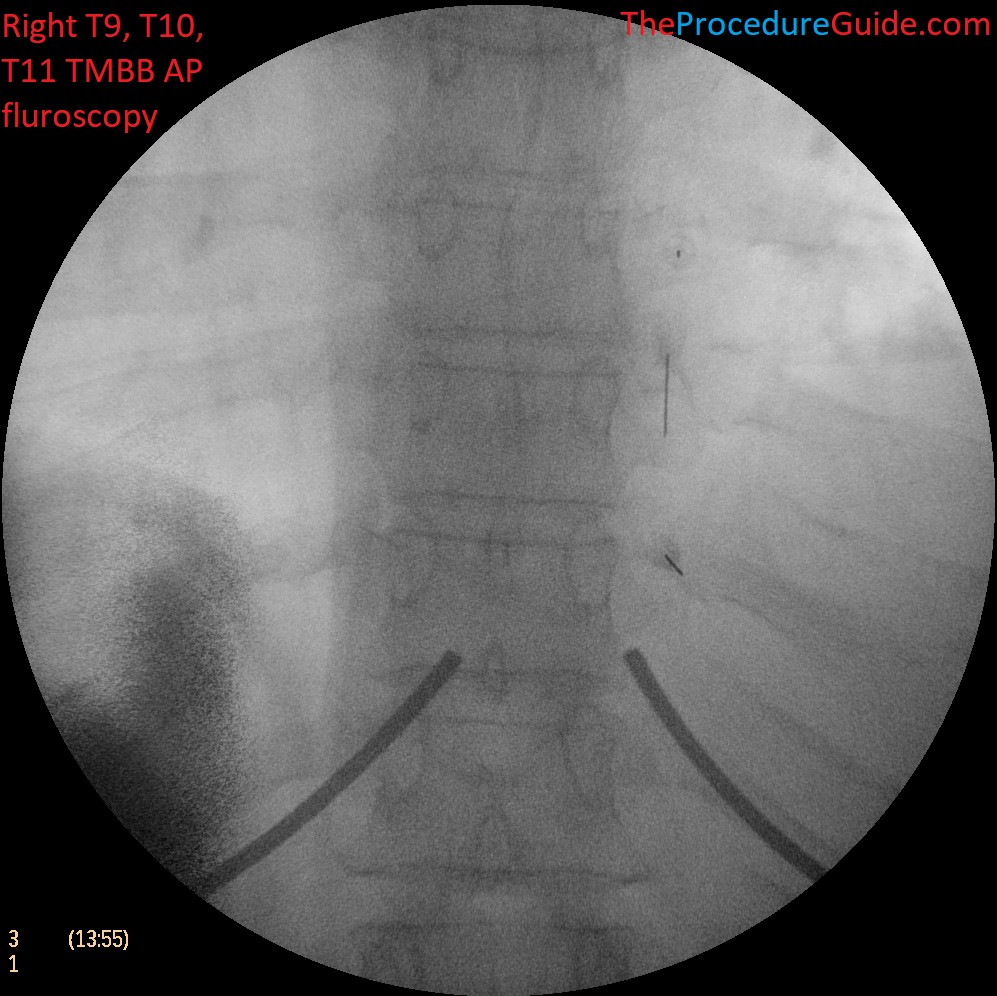
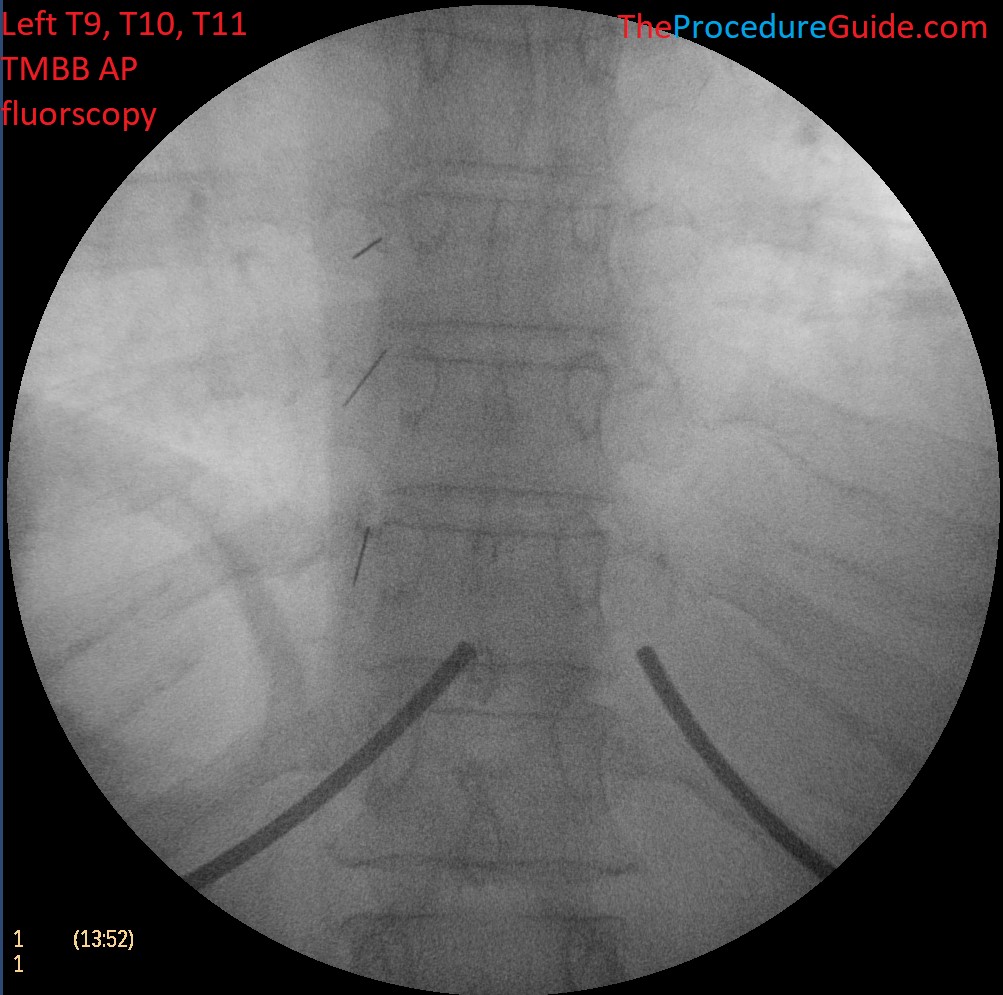
References
Technique Related References
- Percutaneous Radio-Frequency Neurotomy for Chronic Cervical Zygapophyseal-Joint Pain
- Controlled study where a specific two needle technique was used for cervical RF and is described with limited images
- Cervical Medial Branch Radiofrequency Neurotomy in New Zealand
- Some discussion of a two needle technique for cervical RF and is described with limited images.
- Incidence of neuropathic pain after radiofrequency denervation of the third occipital nerve
- Detailed review of variability of third occipital nerve and technique used to ablate it along with some sample images.
General References
- The provocative lumbar facet joint
- Broad and long overview of many clinical aspects of facet anatomy, pathology, treatment studies
- Diagnostic and therapeutic spinal interventions
- Broad overview of medial branch blocks and radiofrequency ablation and discussion of other literature on the topic
- Single needle approach for multiple medial branch blocks: a new technique
- A prospective crossover comparison study of the single-needle and multiple-needle techniques for facet-joint medial branch block
- Radiofrequency lumbar facet denervation: a comparative study of the reproducibility of lesion size after 2 current radiofrequency techniques
