Table of Contents
Name of Procedure
- Thoracic or lumbar medial branch nerve radiofrequency ablation (TRFA or LRFA)
- Neurotomy, rhizotomy, “nerve burn”, RFA
Sample Opnote
The Quick Guide
Goal
To ablate the medial branch nerves that innervate the facet joints of the lumbar or thoracic spine to provide long term relief for facet arthritis.
Indications
Back pain from facet arthritis. Usually non-radicular, over sclerotomal distributions from the affected facet joints.
Contraindications
- Common contraindications
- Posterior fusion at the same levels as the target facet joints (ie, avoid L4-L5 facet treatment in a patient with a fusion at L4-L5) (…)
Anatomy
Overview
A “medial branch” technically refers to the medial branch of the dorsal ramus of a spinal nerve. This medial branch also innervates the multifidus muscle, which is of particular importance when performing a medial branch ablation.
The source/path/naming/innervation of the medial branch nerves and their target injection sites can be confusing so keep a few things in mind:
- Each facet joint is innervated by 2 medial branch nerves. In the lumbar spine, a joint is innervated by a branch from its top level and from the level above it. For example, an L4-L5 facet joint is innervated by a branch from the L3 and L4 spinal nerve.
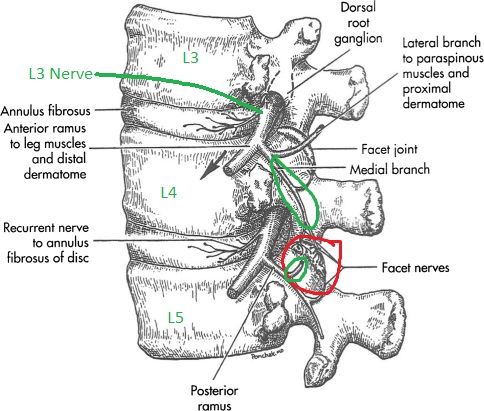
L4-L5 facet in red. L3 and L4 originating branches in green going to innervate that joint.
- The medial branch nerves run over the junction of the transverse process (TP) and superior articulating process (SAP) on the posterior side of the spine, at ONE LEVEL BELOW where it originates.
- See the L3 branch circled in green: to block the medial branch from L3 you target the TP and SAP at L4.
- Note how that branch innervates the L3-L4 joint and continues down to innervate the L4-L5 joint (red). So a block at the L3 level affects two joints.
- Likewise for the branch from L4, you block at L5.
- Now, put together the originating branches and their target sites to determine how to block a specific facet joint:
- To block the medial branch nerves that innervate the L4-L5 facet joint, you would target the junction of the TP and SAP at L4 and again at L5.
- Note this common pattern extends to multiple levels. To block 3 joints (L2-L3, L3-L4, L4-L5), your target sites will be at L2, L3, L4, L5. Note that at L3 and L4, you are getting two half joints at once, which simplifies our procedure.
Naming Notes
The images below use numbering based on the vertebral BODY that is being treated. Ie, a needle on the L4 transverse process is referred to as a L4 MBB target, which is different than the way the nerves would be labeled. This is done to make it easy to follow along with which vertebral bodies are leveled off and targeted.
Equipment/Skills/Setup
Core Equipment/Disposables: See our disposables/equipment article for “core” items that are common to all procedures.
Core Skills: See our guides to obtain images of the cervical, thoracic, or lumbar spine. Then steer a needle to direct it under the skin.
Special items and suggested setup for this procedure:
- RF cannula and probe with RF machine. (2 cannulas and 1 probe will allow for placement of a second cannula, while the prior one is ablating)
- 3cc 1% lidocaine in 3cc syringe
- 10cc 1% lidocaine in 10cc syringe with 25g x 1.5″ hypodermic needle for subcutaneous anesthetic
Landmarks and Patient Positioning
Position the patient in a basic prone position so that the bottom of the c-arm can go under the table below the area of the spine that is being treated.
Technique
For the sake of this tutorial we will assume we are treating the L3-L4, L4-L5, L5-S1 facet joints on one side, which means we have targets at the junction of the SAP and TP at L3, L4, L5, and at the sacral ala.
Background
A radiofrequency ablation is targeting nerves just like a corresponding diagnostic block. But, the key difference is what trajectory the cannula/needle takes to get to the target:
- For a diagnostic block (such as a medial branch block), medication is just being injected, so the tip just has to be close to the target
- The needle can get to the target from anywhere (even at a 90 degree angle to the plane of the target)
- However, a radiofrequency cannula ablates in an oval shaped area parallel to the needle.
- So, if we place the cannula the same as a diagnostic block, the ablation zone may not come in contact with the target as well as if the cannula were lying “flat” over the target area.
- In this diagram, imagine the target is a flat paper at the bottom of the image. If we turned the cannual 90 degrees, then the ablation zone would cover that paper better:
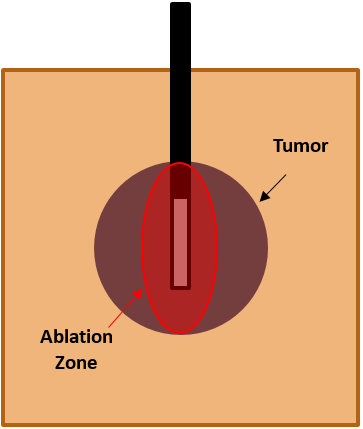
- So, our general approach to RFs is to choose a trajectory that’s as “parallel” to the plane of the target as possible.
Steps
- Obtain an oblique/scotty dog view of L3, which will be the first target.
- Note the different approach from a MBB: The skin entry point for this L3 needle is inferior and lateral to the target site (just lateral to the L2 transverse process).
- Advanced the needle superior and medial till contacting the bone at the inferior border of the L3 transverse process:
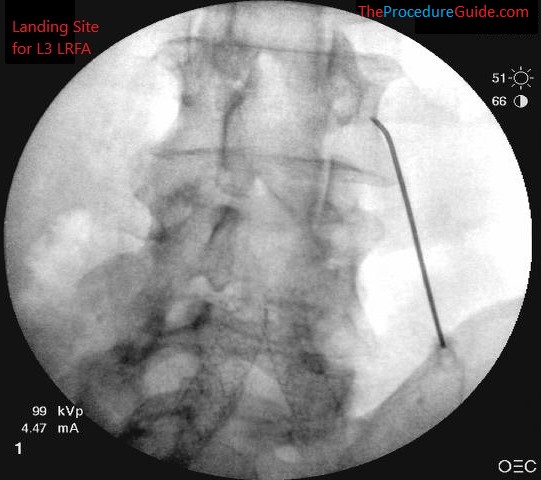
- From here, “slide” the needle along the TP to “lay it flat” over the target site for better RF coverage.
- During this last step of advancing the cannula, inject about 2-3cc of 1% lidocaine to anesthetize the MB nerve so the RF is better tolerated.
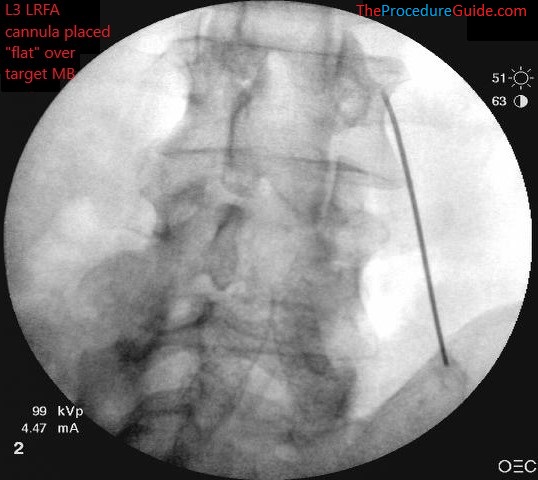
- Confirm your depth positioning on a lateral view
- Confirm that you do not appear to be beyond the transverse process or at the depth of a neuroforamina (not past the blue line below)
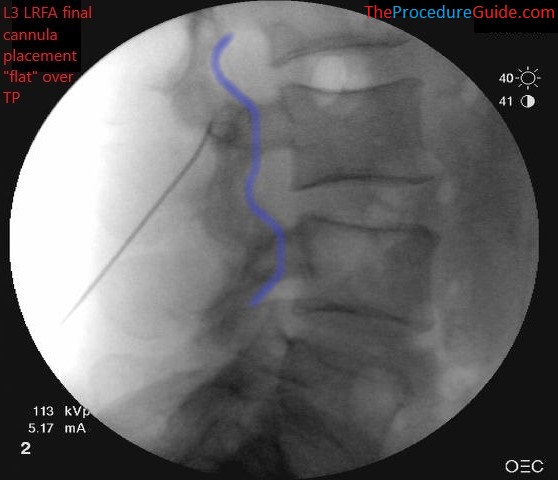
- Perform motor testing after inserting the probe.
- Once negative, ablate.
- During ablation you can restart the above steps to place the second cannula at L4. You can have placement done by the time L3 finishes ablating, and then move the probe L4. This way, the RF machine/ablation is always the rate limiting step.
- This approach allows you to complete a 4 level RF in about 6 minutes.
- Continue repeating the above steps for all levels.
Tips
- There are multiple permutations for how to treat multiple levels, depending on what levels are being treated:
- In the technique described above we are treating L3, L4, L5, sacral ala.
- To do this effectively we place a needle for L3. Then place one for L4. Then place one for the sacral ala. While the sacral ala is being ablated we simply move the L4 needle (which is finished now) to L5.
- This allows for 3 skin entry points and 4 treated levels.
- Most of the times the L5 needle trajectory is sufficient and “flat” enough to work
- You could also do a completely separate entry for L5 for optimal trajectory/needle placement
- For higher levels it’s often necessary to simply do a new entry point for every treated level.
- In the technique described above we are treating L3, L4, L5, sacral ala.
- Placing a needle while prior needles are ablating can help save you time as described above
- Local anesthetic at the target site should be used with caution:
- The steps above call for local anesthetic at the ablation site to help with patient comfort.
- If you don’t get to motor testing right after injection/placement of the needle, the lidocaine can theoretically anesthetize the radicular nerve and give a false negative motor test, which is dangerous.
- To avoid this you can administer local anesthetic after motor testing.
References
Technique Related References
- Percutaneous Radio-Frequency Neurotomy for Chronic Cervical Zygapophyseal-Joint Pain
- Controlled study where a specific two needle technique was used for cervical RF and is described with limited images
- Cervical Medial Branch Radiofrequency Neurotomy in New Zealand
- Some discussion of a two needle technique for cervical RF and is described with limited images.
- Incidence of neuropathic pain after radiofrequency denervation of the third occipital nerve
- Detailed review of variability of third occipital nerve and technique used to ablate it along with some sample images.
General References
- The provocative lumbar facet joint
- Broad and long overview of many clinical aspects of facet anatomy, pathology, treatment studies
- Diagnostic and therapeutic spinal interventions
- Broad overview of medial branch blocks and radiofrequency ablation and discussion of other literature on the topic
- Single needle approach for multiple medial branch blocks: a new technique
- A prospective crossover comparison study of the single-needle and multiple-needle techniques for facet-joint medial branch block
- Radiofrequency lumbar facet denervation: a comparative study of the reproducibility of lesion size after 2 current radiofrequency techniques
